OdySight: Real-World Data Analysis of a Mobile Medical Application for Ophthalmology
Aniket Nikam, Hannah Lefumat, Elidia Grondin, and Vinona Bhatia*
Tilak Healthcare, 74 Rue du Faubourg Saint-Antoine, 75012 Paris, France
Abstract
Digital tools for remote monitoring have revolutionized the current landscape of healthcare delivery. With the advent of smartphones and tablets, the development of mobile medical applications (apps) has created a new dimension in telemedicine. While there are a variety of “wellness apps” available to the general public, only some of them have undergone rigorous human factors testing and clinical validation and require the recommendation of a clinician to be used for remote monitoring. In this article, we specifically review the utility of a mobile medical application called OdySight, which is being recommended by ophthalmologists throughout France for patients with chronic eye diseases.
Introduction
Digital healthcare is attractive to clinicians as a form of telemedicine, to enable and promote patient remote management1,2. The remote monitoring tools embedded within digital healthcare apps3 are uniquely positioned to tackle many current and upcoming challenges4. Digital health companies provide technologies that support the delivery of care virtually and are uniquely suited to expand the capacity of our strained healthcare system4-9. With the COVID-19 public health crisis, the need for remote monitoring tools cannot be over-emphasized4. Hospitals and health systems across the world are witnessing a huge increase in virtual clinic visits, and it's expected that this trend will only continue10. With in-person visits being transitioned to virtual ones11, ophthalmologists are challenged to assess patient health without a physical exam or the imaging technology relied upon in the clinic.
In overburdened hospitals and clinics, worldwide, smartphones and tablets are key to keeping patients out of the clinic when they do not need to be there, and to bring them in, earlier, when they do. For ophthalmology12, in particular, clinical assessment via smartphones13 has existed for several years already14, and teleophthalmology is becoming more popular15,16. There has been a steady rise in the development of home/remote monitoring17-19 systems14,20,21 over the last few years5,22. It has also been suggested that “gamification techniques are likely to increase compliance with self-monitoring, leading to earlier detection in the next generation of patients with neovascular AMD”22-24.
Tilak Healthcare creates mobile medical applications that include a video game with the intent of engaging and entertaining patients, yet require a certain level of commitment and accountability from the patient24,25. Tilak Healthcare’s first app is for the remote monitoring of chronic eye diseases19- the intended use is to assist with the planning of follow up care, between scheduled clinic visits, for patients with age-related macular degeneration, diabetic retinopathy and other similar, treatable causes of blindness. Patients can now use their mobile devices and be active participants in their care, which will hopefully decrease the chance that they will lose their vision prematurely19.
Since September 2018, 152 ophthalmologists across France have recommended OdySight for patients with chronic eye diseases and 950 patients have downloaded the app.
OdySight App
OdySight is designed to monitor clinically relevant visual parameters for patients with chronic eye diseases. OdySight (which comes from the word “odyssée” in French and odyssey in English) was so-named because the player embarks upon an adventure, putting together the pieces of a puzzle with each video game that they play. The patient first completes one, monocular eye test (a digitalized version of Visual acuity or Amsler grid) to boost their “energy” points, allowing them to then play the video game. The puzzle game keeps patients engaged and encourages them to visit the app regularly10,11,13. The patient is limited to a 10-15 minute session each day.
Access and installation of OdySight
In France, the OdySight application is only available by prescription from an ophthalmologist. During a consultation, if the ophthalmologist thinks that OdySight might be useful for a patient, they can create an account for the patient by logging into their clinic dashboard, and completing a form containing the following fields:
• First name of the patient
• Last name of the patient
• Patient’s phone number
• Patient’s email address
• Patient’s visual acuity (for each eye)
• Patient’s eye disease diagnosis (for each eye)
• Patient’s gender
• Patient’s birthdate
After the form is validated by the doctor, the patient receives an email and an SMS containing a link to download the app, as well as a personal code. The clinic staff may assist the patient in installing the app on their device and explain the details of the application. The patient will also receive a small box which contains written instructions for downloading and using the app and contact information for the OdySight support team. The box itself converts into a stand to hold the patient’s phone stationary while they perform visual tests.
After downloading the app, the patient will read and accept the terms of use, enter the personal code they received by SMS/Email, and select a personal password. A short tutorial will show them how to do a test, how to do a puzzle, and how to contact the clinic if an alert is triggered. The patient is completely autonomous and can play the puzzle game and perform visual tests. Each time the patient does a test, their results are automatically displayed on the doctor’s dashboard. If a loss of visual acuity is detected by the OdySight algorithm, the patient and the doctor will be notified and the patient will be encouraged to contact the clinic. The doctor will then decide, according to the data available on the dashboard, to include an additional clinic consultation for the patient, or to have the patient wait until their next scheduled visit.
Medical modules
OdySight currently has two medical modules: 1. Visual acuity; and 2. Amsler Grid; both of which are CE marked and included within the app for the remote monitoring of visual function.
i. Visual acuity module
The Visual Acuity Module is inspired by the standard Early Treatment Diabetic Retinopathy Study (ETDRS) and the “tumbling E” test. It is a short and interactive test during which the patient needs to indicate the orientation of the letter “E” by sliding their finger in the corresponding direction (up, down, left, or right) (Fig. 1 a). Several sizes and orientations of the letter “E” are displayed, one by one, sequentially on the screen. The orientation and the size of the letter changes after each patient's response. The orientation of the letter is random but its size changes according to a predefined algorithm. If the patient does not respond by sliding their finger, then the app will display a button that says “NOT SURE,” and the patient may tap that button. The first time a patient performs the test on each eye, there is an initial screening phase that allows the app to do a ‘threshold’ evaluation of the patient’s visual acuity. Subsequent test sessions will then be much shorter in duration, and more precise based on the patient’s baseline visual acuity. At the end of each test performed, the app displays the patient’s visual acuity test results for that test only. The test stops at the defined threshold for the respective test and this threshold is converted to the corresponding logmar score, which is then translated to the score displayed on the patient’s screen within the app. (eg, logmar 0.0 → decimal value 1.0 → Snellen fraction 10/10 displayed on the app).
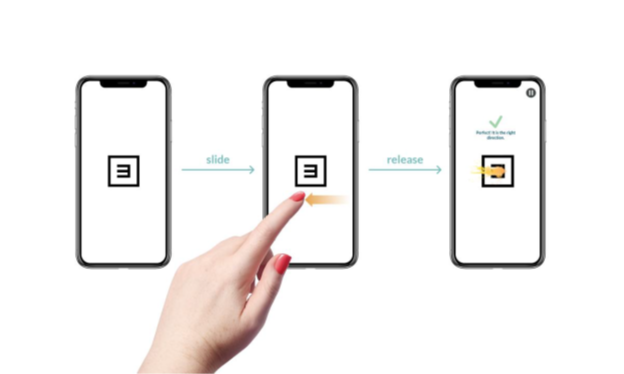
Figure 1. (a): OdySight Visual Acuity Module
When a decrease of the near visual acuity is detected, a pre-alert/alert is triggered, as per the alert algorithm described below.
ii. Amsler grid module
The Amsler Grid Module is a digitalized version of the traditional Amsler grid paper test for the patients who have macular diseases to detect changes in their central vision. In the app, the Amsler grid is displayed in 3 parts on the screen and the patient is required to draw the anomalies they see using their finger instead of a pencil (Fig. 1 b).
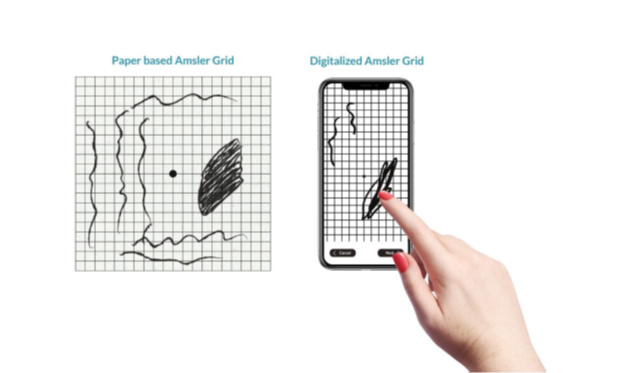
Figure 1. (b): OdySight Amsler Grid Module
There are no alerts with the Amsler grid, but the clinician can visualize the Amsler grid in the dashboard and compare the latest result with the previous tests.
Algorithms for distance to screen and ambient light detection
To ensure that the tests taken using the OdySight modules are precise and reproducible, unique technology (patent filed) has been developed by Tilak Healthcare, including a proprietary algorithm calculating the distance from the patient’s eye to screen and an algorithm for automatic detection of ambient lighting.
In order to continually assess how far the screen is from the patient’s eyes, a special formula is used based on: (i) the interpupillary distance (average or measured on the patient); (ii) the size of the camera feed and current frame; and (iii) the camera properties (sensor physical size, pixel size, and focal-length) for the particular smartphone being used.
To ensure accurate and reproducible test results, the minimum requirement for screen size is 4.7” with dots per inch (DPI) over 260 or even 320 in case one of the eyes has a visual acuity greater than 6/10 (20/32). This recommendation helps to address the impact of different platforms and mobile screen sizes on the score and the repeatability of tests performed on the app.
Algorithm for alerts
Changes in performance for the visual acuity module of OdySight are assessed by an algorithm with a 2-step alert system – if between two tests, there is a change of 5 or more letters in the number of letters correctly identified, then a pre-alert is generated (Fig. 2). The app will automatically prompt the patient to re-do the visual acuity module on the same eye the following day. If, when the visual acuity module is repeated, the user’s performance on that test is the same as the previous day, up to 2 letters better, or worse, then an alert is triggered by the app. In this case, both the patient and clinician (via the secure server and dashboard) will be notified simultaneously that an alert has been triggered. The user is notified by SMS, email, and via the app that they should schedule a visit with their clinician.
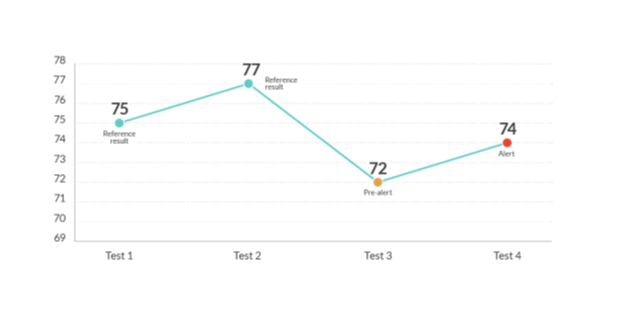
Figure 2: Algorithm for the alert system in OdySight
Limitations and contraindications for OdySight
OdySight is recommended for adults at least 18years of age. It is contraindicated for users who suffer from epilepsy or seizures and for those with:
i. Binocular vision worse than logMAR 0.5 (20/63).
ii. No access to a compatible smartphone and/or tablet.
iii. No valid email address or phone number which are required to create an account and receive alerts.
iv. A lack of competence to use the app and complete the test modules remotely, without the guidance of a clinician.
Clinical Validation of OdySight
Overview
The framework under which digital therapies need to be designed is not too different from how traditional medications are studied and tested. Clinical validation of the modules of OdySight was therefore undertaken with 122 eyes (88 patients) in France in 201819,25.
TIL-001 clinical trial summary
The clinical study was designed to evaluate OdySight’s medical modules by comparing them directly to the gold standard tests for visual acuity, contrast sensitivity, and Amsler Grid. The results of this study demonstrate good agreement with statistical significance, for the measurements taken by two of OdySight’s medical modules (visual acuity and Amsler grid) when compared to present-day gold standards (ETDRS Sloan near visual and distance ETDRS charts and paper Amsler Grid, respectively) (Fig. 3) in the majority of the study population19. OdySight was validated to be a good alternative to traditional clinical tests and a powerful tool for remote monitoring of vision between clinic visits, and could potentially assist in follow-up planning.
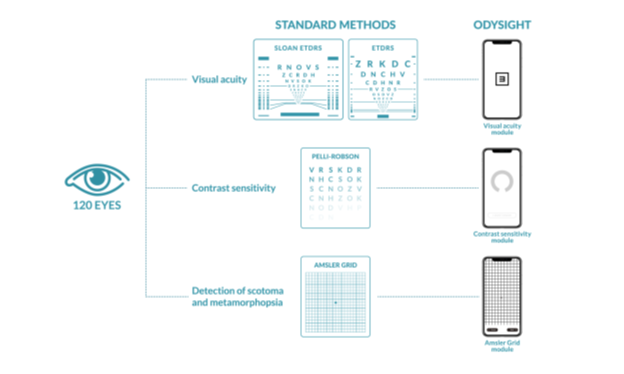
Figure 3: Evaluation of OdySight medical modules compared to Gold standard tests
The study is similar to the results from other studies16,17,21 in which remote monitoring apps were validated and to those that compared apps with existing gold standard tests21,22,26.
Real-World Use of OdySight
OdySight users based on eye disease
OdySight has been most commonly recommended for patients with a diagnosis of wet age-related macular degeneration (AMD) (35% of all patient downloads) (Fig. 4). Similarly, the cohort with the most active players are patients with wet AMD. (Fig. 4). Non-players are defined as those who did fewer than three sessions (performing eye tests or doing puzzles) or fewer than three puzzles, or those for whom the number of puzzles completed is less than 10% of their total number of sessions.
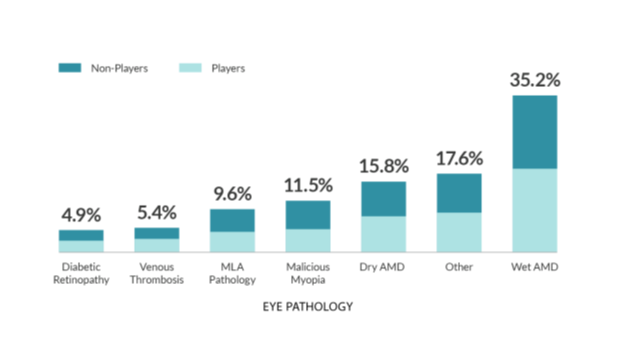
Figure 4: Eye Pathology among total OdySight user population in France by player/non-player profile
OdySight users based on age
Age cohort-based distribution among OdySight users reveals that the most frequent users are in the age cohort of 70-80 years, with the maximum number of players (vs non-players) also being in this cohort (Fig. 5). Overall, the maximum number of users are in the age range of 50-80. And, interestingly, even in the age cohort of >80 years, comprising 17.6% of the patient population, more than 50% of the cohort is defined as players (Fig. 5).
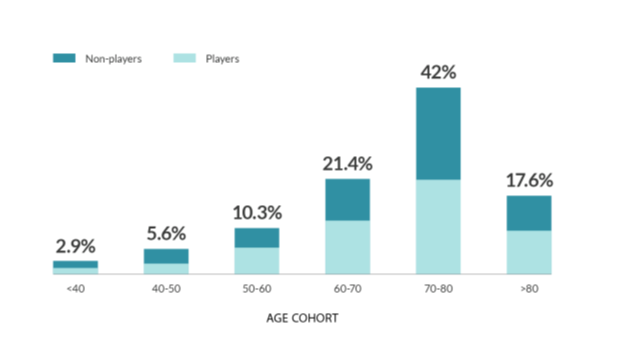
Figure 5: Age group cohorts among total OdySight user population in France by player/non-player profile
Retention rates based on age
Retention is a key component to the success of mobile technology. When the patient becomes bored or fatigued by a mobile application or game, they will likely stop being engaged and rarely restart gameplay again. The mobile applications with the best retention on the market are Instagram (70%) and WhatsApp (62%). OdySight has average retention of 43% for three months (Fig. 6 a). Patients who play the game regularly have the best retention (defined by the number of patients who use the application at least once over the given period). Also, it is worth noting that players have much better retention than non-players (63% vs 17% at three months) (Fig. 6 a).
Remarkably, patients in the age group, 80+ years, have three-month retention of 43% (53% for the age group 65-80 years) (Fig. 6 b).
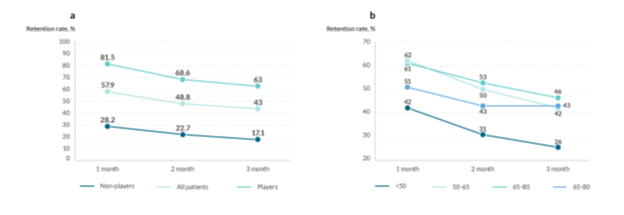
Figure 6: Retention rates among OdySight user population in France; (a) by total population and player/non-player profile; (b) by age
Summary
OdySight was developed to address the growing need for remote monitoring of visual function among patients suffering from AMD and other chronic eye diseases. As a mobile medical application, it is simple for clinicians to recommend during a patient visit and for patients to download and use the app remotely. OdySight has shown good retention in all age groups analyzed and, particularly, in elderly patients. Players demonstrate better retention which implies that the puzzle game keeps patients interested and engaged (Fig. 7).
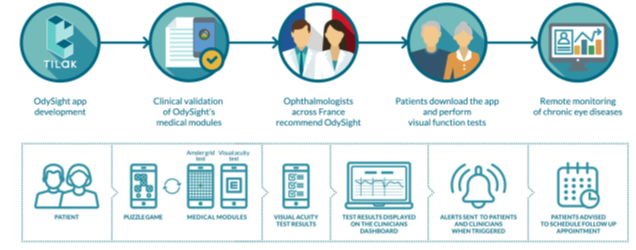
Figure 7: OdySight: A mobile medical app for the remote monitoring of vision
The Future of OdySight
The value of mobile, remote monitoring comes from an accurate alert system. Tilak is now planning a randomized controlled trial to assess the sensitivity and specificity of the unique alert algorithm of OdySight. OdySight is now available in the Apple and Android application stores in France and the US for free download and a 30-day trial. A clinician must provide a code to the patient for data exchange to occur and to allow the use of the app for more than 30 days. Tilak Healthcare’s second mobile medical application will be for mental health disorders, particularly addiction.
References
- Bradbury K, Watts S, Arden-Close E, et al. Developing Digital Interventions: A Methodological Guide. Evidence-Based Complementary and Alternative Medicine. 2014. https://www.hindawi.com/journals/ecam/2014/561320/ doi:https://doi.org/10.1155/2014/561320.
- Wanless D. Securing our Future Health: Taking a Long-Term View. 179.
- Jarry O. Council Post: How To Gain A Foothold In The Digital Therapeutics Industry. Forbes https://www.forbes.com/sites/forbesbusinessdevelopmentcouncil/2020/03/25/how-to-gain-a-foothold-in-the-digital-therapeutics-industry/.
- Smith AC, Thomas E, Snoswell CL, et al. Telehealth for global emergencies: Implications for coronavirus disease 2019 (COVID-19). J Telemed Telecare. 2020. 1357633X2091656 doi:10.1177/1357633X20916567.
- Vegesna A, Tran M, Angelaccio M, et al. Remote Patient Monitoring via Non-Invasive Digital Technologies: A Systematic Review. Telemed E-Health. 2017; 23: 3–17.
- Digital therapeutics: An exciting innovation, but not without challenges. Roland Berger https://www.rolandberger.com/de/Point-of-View/Digital-therapeutics-An-exciting-innovation-but-not-without-challenges.html.
- Providence St. Joseph using Twistle remote monitoring technology for 700 COVID patients. FierceHealthcare https://www.fiercehealthcare.com/tech/providence-using-twistle-remote-monitoring-technology-for-700-covid-patients.
- More ACOs turn to telehealth to combat COVID-19 financial crisis. FierceHealthcare https://www.fiercehealthcare.com/hospitals-health-systems/more-acos-turn-to-telehealth-to-combat-covid-19-financial-crisis.
- Zocdoc, startups expanding telehealth offerings to meet demand. FierceHealthcare https://www.fiercehealthcare.com/tech/zocdoc-adds-telehealth-appointments-to-platform-to-help-meet-spike-demand-for-virtual-care.
- Mehrotra Ateev, Ray Kristin, Brockmeyer Diane M, et al. Rapidly Converting to “Virtual Practices”: Outpatient Care in the Era of Covid-19. Catal. Non-Issue Content 1.
- Playing to Win Patient Engagement | HealthLeaders Media. https://www.healthleadersmedia.com/strategy/playing-win-patient-engagement.
- Akkara. Innovative smartphone apps for ophthalmologists. http://www.kjophthal.com/article.asp?issn=0976-6677;year=2018;volume=30;issue=2;spage=138;epage=144;aulast=Akkara.
- Chhablani J, Kaja S, Shah VA. Smartphones in ophthalmology. Indian J Ophthalmol. 2012; 60: 127–131.
- Mohammadpour M, Heidari Z, Mirghorbani M, et al. Smartphones tele-ophthalmology and VISION 2020. Int J Ophthalmol. 2017; 10: 1909–1918.
- Zvornicanin E, Zvornicanin J, Hadziefendic B. The Use of Smart phones in Ophthalmology. Acta Inform Medica. 2014; 22: 206–209.
- AREDS2-HOME Study Research Group et al. Randomized trial of a home monitoring system for early detection of choroidal neovascularization home monitoring of the Eye (HOME) study. Ophthalmology. 2014; 121: 535–544.
- Han X, Scheetz J, Keel S, et al. Development and Validation of a Smartphone-Based Visual Acuity Test (Vision at Home). Transl Vis Sci Technol. 2019; 8.
- Karthikeyan SK, Thangarajan R, Theruvedhi N, et al. Android mobile applications in eye care. Oman J Ophthalmol. 2019; 12: 73–77.
- Brucker J, Bhatia V, Sahel JA, et al. Odysight: A Mobile Medical Application Designed for Remote Monitoring—A Prospective Study Comparison with Standard Clinical Eye Tests. Ophthalmol Ther. 2019; 8: 461–476.
- Martínez-Pérez B, de la Torre-Díez I, López-Coronado M. Mobile health applications for the most prevalent conditions by the World Health Organization: review and analysis. J Med Internet Res. 2013; 15: e120.
- Wang YZ, He YG, Mitzel G, et al. Handheld Shape Discrimination Hyperacuity Test on a Mobile Device for Remote Monitoring of Visual Function in Maculopathy. Invest Ophthalmol Vis Sci. 2013; 54: 5497–5505.
- Razavi H, Baglin E, Sharangan P, et al. Gaming to improve vision: 21st century self-monitoring for patients with age-related macular degeneration. Clin Experiment Ophthalmol. 2018; 46: 480–484.
- How to Use Gamification to Improve Patient Engagement and Adherence. HealthPrize Technologies. 2018. https://healthprize.com/blog/gamification-to-improve-patient-engagement-adherence/
- Odysight - Tilak Healthcare. https://www.tilakhealthcare.com/en/home/.
- Tilak Healthcare Publishes Its First Clinical Trial, TIL-001. 2019. https://www.businesswire.com/news/home/20190905005395/en/Tilak-Healthcare-Publishes-Clinical-Trial-TIL-001.
- Perera C, Chakrabarti R, Islam FMA, et al. The Eye Phone Study: reliability and accuracy of assessing Snellen visual acuity using smartphone technology. Eye Lond Engl. 2015; 29: 888–894.
